Most Missed Peds EM Exam Prep - Decompression Sickness Transport
PEM board review: severe decompression sickness needs hyperbaric transfer with 100% O2 and minimal altitude exposure—pressurized fixed-wing is...
Adolescent anterior tibial tubercle pain suggests Osgood-Schlatter. Treat with NSAIDs/ice, activity modification, and quad/hamstring stretching.
Key takeaway: Adolescent anterior tibial tubercle pain from Osgood–Schlatter is treated with pain control plus *activity modification and flexibility/strengthening*, not routine immobilization or advanced imaging.
A 12 yo boy presents to the ED with anterior left knee pain. He has been having pain on-and-off for several weeks, beginning when he started playing basketball for his school team. Yesterday, the pain was worse, and he had to sit out of a game, which his father states is unusual for him. He denies any specific injury, and he denies any “pops” or feeling of instability in the knee. He took ibuprofen prior to arrival, and this helped alleviate some of the pain. He has not tried any other treatment modalities. On exam, he has point tenderness on the proximal anterior tibia in the midline of the lower leg. He has no edema of the knee itself, and the knee is grossly stable. He has no pain with internal and external rotation of the hip. He ambulates normally but states it will hurt to run or jump. The following radiograph is obtained.
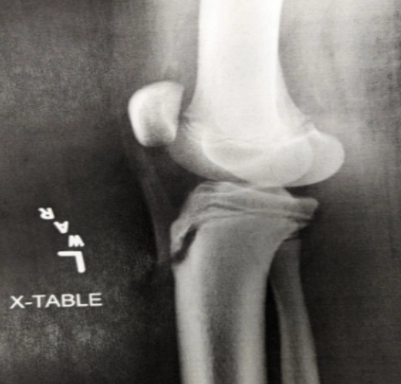
Image by exclusive permission of personal collection of Ashley Barrile, M.D. All rights reserved
Which of the following is the best treatment strategy?
Answer Options:
In this item, the keyed answer (A) is directionally aligned with current standard management (conservative care with symptom control and stretching/rehab, with relative activity modification rather than mandatory cessation). However, the explanation’s “24-hour” rule is not a universally stated guideline threshold; major references (e.g., AAOS OrthoInfo and UpToDate updates within the last decade) emphasize pain-guided activity modification and gradual return rather than a strict time-based cutoff.
That said, among the provided options, A remains the best answer because it includes the full conservative package clinicians are expected to recognize for boards: ice/NSAIDs + quadriceps/hamstring stretching (often via PT/HEP) + continued participation as tolerated with modification. Option D is close, but it frames management as “restrict” from painful activities without explicitly incorporating the rehab component that is central to recovery and recurrence prevention.
| Option | What It Tests / Implies | Why It’s Wrong Here |
| A. | Conservative care + activity as tolerated + flexibility rehab | Best match to guideline-consensus management for Osgood–Schlatter (AAOS/UpToDate). The “24 hours” framing is extra, but the overall strategy is correct. |
| B. | Concern for occult tibial plateau fracture needing CT | No acute trauma, no effusion/instability, and exam localizes to tibial tubercle region; CT is not indicated for classic traction apophysitis. |
| C. | Immobilization and ortho follow-up as if ligament/meniscus/patellar instability | Routine knee immobilizer is not standard for Osgood–Schlatter; may worsen stiffness/deconditioning and is reserved for certain acute injuries or severe cases under specialist guidance. |
| D. | Pure activity restriction + symptomatic care | Too narrow: activity modification is appropriate, but comprehensive management typically includes stretching/strengthening (often PT) to address tight quads/hamstrings and biomechanics. |
Osgood–Schlatter = tibial tubercle traction apophysitis treated with ice/NSAIDs + stretching/strengthening and **relative rest/activity modification**, not immobilization or advanced imaging.
The stem pushes you toward “something structural” (radiograph + point tenderness) and tempts over-management (CT, immobilizer). Boards reward recognizing the classic overuse pattern (weeks of activity-related anterior tibial tubercle pain, stable knee, no acute injury) and choosing conservative, rehab-forward care with pain-guided activity modification.
A 13-year-old soccer player has 6 weeks of anterior knee pain localized to the tibial tubercle, worse with jumping, improved with rest. Knee is stable; no effusion; X-ray shows fragmented tibial tubercle apophysis. Best initial management?
A — Review: Casting/immobilization is not routine for uncomplicated Osgood–Schlatter.
B — Correct response!: First-line conservative care: pain control + relative rest + flexibility/rehab (AAOS/UpToDate-consensus).
C — Review: Advanced imaging not indicated without acute trauma/red flags.
D — Review: Surgery is rare and reserved for refractory, usually skeletally mature cases.
E — Review: Overly restrictive; return is typically guided by symptoms with modification.
A 12-year-old basketball player has anterior knee pain. Today he felt a “pop” during takeoff and now cannot extend the knee against gravity; there is a large effusion. Next best step?
A — Review: Red flags (pop, extensor lag, effusion) suggest acute injury.
B — Review: Unsafe with suspected extensor mechanism disruption.
C — Correct response!: Acute extensor mechanism injury requires immobilization and urgent evaluation.
D — Review: This is not typical Osgood–Schlatter.
E — Review: Imaging choice depends on suspected injury; CT is not universal first-line.
A 14-year-old with Osgood–Schlatter asks if he must stop all sports. Best counseling?
A — Review: Too strict; most improve with conservative care and modification.
B — Correct response!: Pain-guided modification/relative rest is standard (AAOS/UpToDate).
C — Review: Ignoring pain can worsen symptoms and prolong recovery.
D — Review: Opioids are not appropriate for this condition.
E — Review: Surgery is rarely indicated.
Which finding most supports Osgood–Schlatter over patellar tendon rupture?
A — Review: Suggests acute injury.
B — Correct response!: Chronic overuse + tibial tubercle tenderness is classic.
C — Review: Suggests extensor mechanism disruption.
D — Review: Patella alta suggests patellar tendon rupture.
E — Review: Hemarthrosis suggests intra-articular injury.
A 13-year-old with Osgood–Schlatter has persistent pain despite NSAIDs and basic stretching. Next best step?
A — Review: Not indicated without concern for fracture/other pathology.
B — Correct response!: Escalate conservative therapy with PT/adjuncts commonly recommended in consensus resources.
C — Review: Not a first- or second-line approach.
D — Review: Noninfectious overuse condition.
E — Review: Overly restrictive for typical disease.
How would your workup and disposition differ between (1) classic Osgood–Schlatter symptoms over weeks with stable knee and (2) sudden anterior knee pain after a jump with extensor lag and effusion?
A: Usually no—ABP/PEM-style exams expect recognition based on history/exam; plain radiographs may be used to rule out other pathology when uncertain, but advanced imaging is uncommon without red flags.
A: No—exam standards align with relative rest/activity modification guided by pain plus rehab (AAOS/UpToDate consensus).
A: Not for uncomplicated Osgood–Schlatter; immobilization is reserved for suspected acute structural injury (e.g., extensor mechanism injury) or select severe cases under specialist direction.
A: Stretching/strengthening (especially quadriceps/hamstrings, and overall biomechanics) plus gradual return to activity—this is what differentiates optimal care from “just NSAIDs.”
Find this and other Pediatric Emergency Medicine exam prep questions in Med-Challenger Pediatric Emergency Medicine 3rd Edition Exam Review with CME
Try for free and save. Ace your exams and meet your CME/MOC requirements.
No matter your program, no matter the size, Med-Challenger for Groups and Institutions can better prepare your program or group, fulfill industry requirements, and increase test scores.
PEM board review: severe decompression sickness needs hyperbaric transfer with 100% O2 and minimal altitude exposure—pressurized fixed-wing is...
PEM board-style Most Missed Question: post‑intubation CXR interpretation and ET‑tube positioning in a 13‑y/o with myotonic dystrophy.
In pediatric trauma with suspected C-spine injury, start with a jaw thrust; if ineffective, proceed to head tilt–chin lift. Cricoid pressure is not...
Stay informed of new medical education content, certification requirements and deadlines, case-based CME quizzes, and special offers.